Embrace greater efficiencies
after PFA
Perclose™ Devices are the only vascular closure
devices approved to close after all
Pulsed Field Ablation (PFA) Systems §,1,†

Perclose™ ProStyle™ Suture-Mediated Closure for EP Ablation Procedures
ENABLE immediate and durable hemostasis1 with >96% freedom from major access site related complications at 30 days2,3,4,5
ENHANCE your patient's comfort and satisfaction over manual compression1,5,17
EMPOWER higher EP lab efficiency with ambulation in as early as 2 hours1,2,4* and same day discharge2,3,4,5**
Learn more about how you can finish your procedure with confidence.

Enable Immediate and Durable Hemostasis Through Suture-Mediated Repair
The Perclose™ ProStyle™ closure device achieves rapid hemostasis of femoral access sites by approximating the edges of the vessel wall with a surgical suture. The benefits of suture-mediated repair include promoting primary intention healing with less scarring18 and decreased time to hemostasis, ambulation, and patient discharge.4,19
Suture-Mediated Repair with Perclose™ ProStyle™
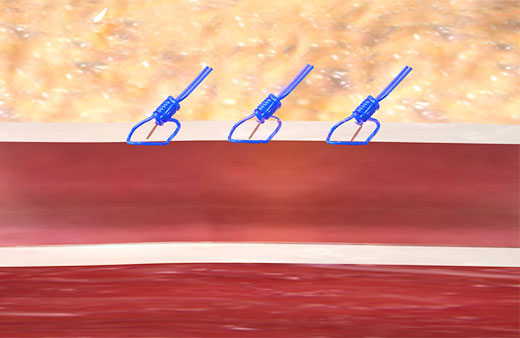
Unlike collagen based VCDs,† Perclose™ Prostyle™ has no re-access restrictions.1
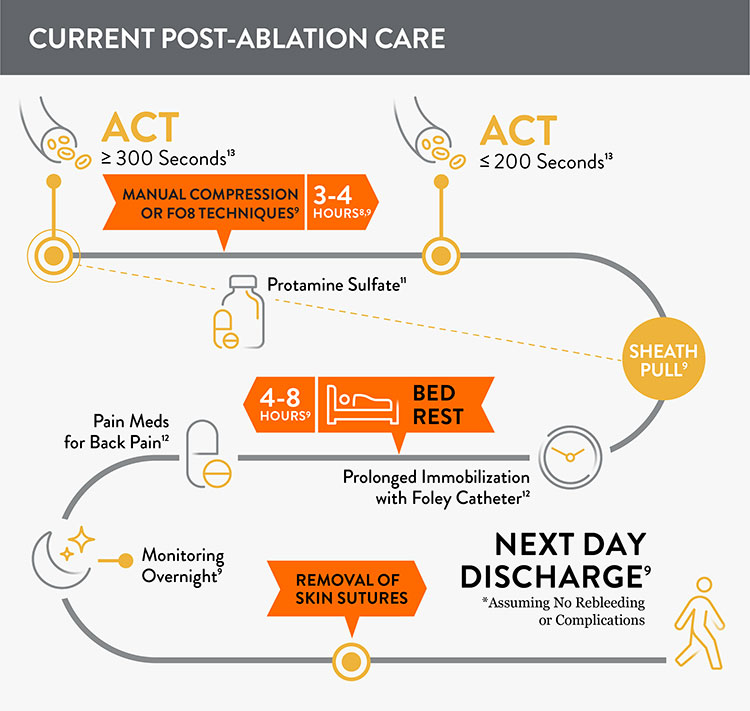
Before: More Closure-Related Interventions Mean More Staff Time
Prior to adopting Perclose™ ProStyle™ SMCR System, EPs completing an atrial fibrillation ablation or other procedures may find that patients require:
- Multiple venous sheaths and access sites8
- Uninterrupted anticoagulation: activated clotting time (ACT) ≥ 300 seconds9,10
- Manual compression at groin access site for up to 30 minutes9
- Protamine sulfate to reverse the effects of heparin11
- Figure-of-eight (FO8) to maintain hemostasis9
- Prolonged immobilization/bedrest of 4-12 hours to prevent bleeding and complications9
- A Foley catheter12
- Discharge 249-7210 hours after the procedure
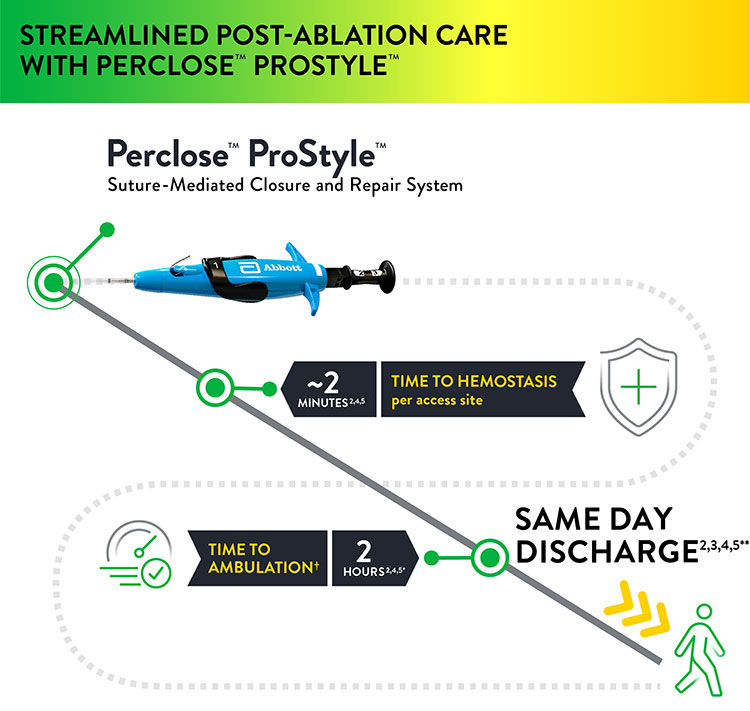
Using Perclose™ ProStyle™ Device: Improved EP Lab Workflow, Enhanced Patient Experience
The Perclose™ ProStyle™ closure device transforms an otherwise lengthy patient recovery to a shorter recovery time, which in turn leads to a positive patient experience:
- Time to hemostasis (TTH) on avg is ~2 minutes per access site2,4,5
- Patient may sit up immediately; no lay-flat restrictions1
- Patients can ambulate after 2 hours1
- Patient may be eligible for same-day discharge2,3,4,5**
The STYLE-AF (randomized two-arm study, n=125) compared Perclose™ Systems to Figure-of-Eight sutures after PFA, and Cryo ablations for Afib. The Perclose™ Study group demonstrated a significantly reduced hemostasis, ambulation, and discharge eligibility times and increased patient satisfaction with their bedrest time relative to the Fo8 control group.26

Empower Higher EP Lab Efficiency, Lower Avoidable Costs, and Improve Patient Experience
1,000+ patients have demonstrated the safety and effectiveness of Perclose™ ProStyle™ in closing multiple CFV access sites across multiple real-world investigator sponsored studies (ISS).2,3,4,5,24,25,26
The use of Perclose™ ProStyle™ Suture-Mediated Closure and Repair System can help:

SOURCE: S. Verma. Adopting a Strategy of Early Ambulation and Same-Day Discharge for Atrial Fibrillation Ablation Cases - EP Lab Digest - May 2019.

Case Recordings
Each of these brief videos offers details of multiple device deployment using Perclose™ closure devices.
AFib RF Ablation with
4x Venous Access Sites
Brett Gidney, MD
Santa Barbara, U.S.
AFib RF Ablation with
4x Venous Access Sites
Hemanth Ramanna, MD
The Hague, The Netherlands
2x Large-Bore Vascular Closure
Magnus Settergren, MD
Solna, Sweden
More case video recordings are available, with physicians offering additional details about their use of the Perclose ProGlide™ device.
Can Perclose™ ProStyle™ be used for vascular closure after Pulsed Field Ablation (PFA) for AFib?
Yes, Perclose™ ProStyle™ can be used in conjunction with a variety of AFib ablation techniques, including Pulsed Field Ablation (PFA) for venous sheaths up to 24F ID (29 OD).1†
At the time of this publication, only Perclose™ Devices can close after all PFA systems including Farapulse‡ (13F Inner Diameter (ID), 16.8F Outer Diameter (OD)). §,1,†
Why would I want to use a vessel closure device (VCD) in a vein?
Using a VCD has several advantages given the following factors during EP procedures such as AF ablations:
- Physicians often have multiple access sites to manage, even some involving large caliber venous sheaths.8
- Patients often receive full-dose peri-procedural anticoagulation, and this can make complete hemostasis a challenging and lengthy process, requiring prolonged immobilization.9,10
- The typical EP lab post-procedure process requires the patient to remain immobilized for prolonged periods of time, which is a source of patient discomfort.9
All of these issues are mitigated when using the Perclose™ ProStyle™ closure device.
Is Same-Day Discharge after AF ablations safe?
Yes, Same-Day Discharge has been shown to be safe, and it is being used to reduce the total cost of care and to enhance the patient experience. The use of vessel closure devices makes it possible for hospitals to implement Same-Day Discharge.4,17,20,21
What makes Perclose™ ProStyle™ SMCR System different from other vascular closure devices?
With the Perclose™ ProStyle™ device you can achieve and confirm complete hemostasis on the table with a suture-mediated repair of the access site. Other advantages of the Perclose ProGlide™ SMC System include:
- The broadest indication† for use in both common femoral veins and arteries
- No ACT-level requirements, so reversal of heparin is not required in order to achieve immediate and durable hemostasis1,13
Find out more about primary healing with the Perclose ProStyle™ vessel closure device.
For what range of sheath sizes and devices can the Perclose™ ProStyle™ SMCR System be used?
Does the Perclose™ ProStyle™ device come in different sizes?
No, there is only one Perclose™ ProStyle™ SMCR System. Multiple Perclose™ ProStyle™ devices can be used, if necessary, for large-bore vascular closure.
How quickly can a patient be mobilized, ambulated, and discharged when using the Perclose™ ProStyle™ closure device?
Because this device achieves immediate and durable hemostasis, patients may sit up immediately in bed.1 Clinical evidence for cardiac arrhythmia treatments with multiple access sites has shown that patients safely ambulated within 2 hours2,4,5,* and were eligible for same-day discharge after successfully closing with Perclose™ devices.2,3,4,5**
How does the Perclose™ ProStyle™ SMCR System achieve immediate and durable hemostasis?
It achieves hemostasis by approximating the edges of the vessel wall with a surgical suture, allowing primary intention healing to begin. Primary intention healing minimizes scarring and allows for immediate reaccess if needed. View primary intention healing images with vessel closure device.18
What kind of training is available to begin using the Perclose™ ProStyle™ SMCR System?
Contact your local Abbott representative for a training opportunity.
What is the "Pre-Close" Technique?
The "Pre-Close" Technique involves the Perclose™ ProStyle™ suture being placed around the access site before the index procedure, and it is required before using sheath sizes > 8F.1
See Deployment and Instructions for Use for additional information.
Visit the official Perclose™ ProStyle™ website for more information on the features, deployment, clinical data, Perclose™ ProStyle™ videos, and ordering information related to Perclose™ ProStyle™ SMCR System.
References
§ At the time of this publication (Oct 2024), for the following PFA systems: Farapulse‡# (13F Inner Diameter (ID), 16.8F Outer Diameter (OD)), PulseSelect‡ (9.5F ID; 14F OD), and Varipulse‡ (8.5F ID; 11.5 OD)
†As compared to Angio-Seal‡, ExoSeal‡, Celt ACD‡, MANTA‡, Mynx‡, Vascade‡. Data on file at Abbott.
*As observed in the VACCAR trial (≥1.4 hours) and the PRO-PVI trial (≥1:26 time to ambulation) after successful close with Perclose device(s) in patients who have undergone cardiac arrhythmia treatments with multiple common femoral venous access sites.
**As observed in the PROFA trial (80% discharged within 3:34h) and the PRO-PVI trial (≥3:38 hours post-procedural time to discharge) after successful close with Perclose device(s) in patients who have undergone cardiac arrhythmia treatments with multiple common femoral venous access sites.
- Perclose™ ProStyle™ Suture-Mediated Closure and Repair (SMCR) System Instructions for Use (IFU). Refer to IFU for additional information.
- Mohammed et al (2022) Comparative outcomes of vascular access closure methods following atrial fibrillation. Vascular Closure for Cardiac Ablation Registry. (VACCAR) J Interv Card Electrophysiol 64, 301 -310
- Castro-Urda et al (2023) Efficacy and safety of Proglide use and early discharge after atrial fibrillation (PROFA trial) Pacing and Clinical Electrophysiology, 46(7), 598-606.
- Fabbricatore D et al. (2023) Ambulatory PV isolation workflow using suture-mediated vascular closure devices: a prospective observational cohort study. (PRO-PVI Study). Europace. 25(4):1361-1368
- Kiani S et al. (2022) Percutaneous Vascular Closure Compared with Manual Compression in AF Ablation. JACC JACC. Clinical electrophysiology, 8(6), 803 -805. (ESM trial)
- Sekhar A, et al. Femoral arterial closure using ProGlide™ is more efficacious and cost-effective when ambulating early following cardiac catheterization. Int J Cardiol Heart Vasc. 2016;13:6-13. doi: 10.1016/j.ijcha.2016.09.002.
- 20 million+ closures based on July 2024 Finance Report. Data on file at Abbott.
- Gupta S. I Just Need Some Closure: Getting Past Using Manual Compression After Ablation. HRS 2018.
- Lakshmanadoss U, et al. Figure-of-eight suture for venous hemostasis in fully anticoagulated patients after atrial fibrillation catheter ablation. Indian Pacing Electrophysiol J. 2017;17:134-139. doi: 10.1016/j.ipej.2017.02.003
- Okada M, et al. Efficacy and safety of figure-of-eight suture for hemostasis after RFCA for AF. Circ J. 2018;82:956-964. doi: 10.1253/circj.CJ-17-1213.
- Ghannam M, et al. Protamine to expedite vascular hemostasis after catheter ablation of atrial fibrillation: A randomized controlled trial. Heart Rhythm. 2018;15(11):1642-1647. doi: 10.1016/j.hrthm.2018.06.045.
- Mohanty S, et al. Venous access-site closure with vascular closure device vs. manual compression in patients undergoing catheter ablation or left atrial appendage occlusion under uninterrupted anticoagulation. EP Europace. 2019;21:1048-1054. doi.org/10.1093/europace/euz004.
- Calkins H, et al. 2017 HRS/EHRA/ECAS/APHRS/SOLAECE expert consensus statement on catheter and surgical ablation of atrial fibrillation. Heart Rhythm. 2017;14(10):e275-e444. http://dx.doi.org/10.1016/j.hrthm.2017.05.012.
- Kar, S., et al, The Use of Perclose ProGlide Suture-Mediated Closure (SMC) Device for Venous Access-Site Closure Up to 24F Sheaths. CRT 2018.
- Mahadaven VS, et al. Pre-closure of femoral venous access sites used for large-sized sheath insertion with the Perclose device in adults undergoing cardiac intervention. Heart. 2008;94:571-572. doi.org/10.1136/hrt.2006.095935.
- Sairaku A, et al. Rapid hemostasis at the femoral venous access site using a novel hemostatic pad containing kaolin after atrial fibrillation ablation. J Interv Card Electrophysiol. 2011;31:157-164.
- Verma S. Adopting a strategy of early ambulation and same-day discharge for atrial fibrillation ablation cases. EP Lab Digest. 2019;19(5).
- Mercandetti M. Wound Healing and Repair. Medscape. Accessed March 1, 2024. https://emedicine.medscape.com/article/1298129-overview
- Bhatt DL, et al. Successful “pre-closure" of 7Fr and 8Fr femoral arteriotomies with a 6Fr suture-based device (the Multicenter Interventional Closer Registry). Am J Cardiol. 2002;89:777-779.
- Bartoletti S, Mann M, Gupta A, et al. Same‐day discharge in selected patients undergoing atrial fibrillation ablation. Pacing Clin Electrophysiol. 2019;42:1448-1455.
- Deyell M, Macle L, Khairy P, et al. The efficacy of a same-day discharge protocol after atrial fibrillation ablation. Canadian J Cardiol. 2018;34:(10 suppl):S84. doi:https://doi.org/10.1016/j.cjca.2018.07.281.
- Data on file at Abbott.
- Verma, S., et al, Feasibility and Safety of Same Day Discharge for Patients Undergoing Atrial Fibrillation (AF) Ablation in a Community Hospital Setting. HRS 2020 Science Online, May 2020.
- Sun, J. Y., et al. (2023). Feasibility and clinical benefits of the double-ProGlide technique for hemostasis after cryoballoon atrial fibrillation ablation with uninterrupted oral anticoagulants. Journal of geriatric cardiology : JGC, 20(4), 268–275.
- Ahmed, A, Bawa, D, Kabra, R. et al. EFFICACY OF VENOUS CLOSURE METHODS AFTER ELECTROPHYSIOLOGICAL PROCEDURES. J Am Coll Cardiol. 2023 Mar, 81 (8_Supplement) 147.
- Richard Tilz, R et al (2024) Venous Vascular Closure System Versus Manual Compression Following Single Shot Device AF Ablation -The STYLE-AF Study
MAT-2002002 v9.0