The XACT™ Carotid Stent System and XACT™ Transcarotid Stent System
Designed to deliver precision, strength, and performance for carotid artery stenting (CAS), offering both transfemoral and transcarotid (TCAR) delivery options.
Backed by five clinical studies and registries, with over 10,000 patients treated, XACT™ has demonstrated proven low stroke rates1 and consistent long-term vessel patency.
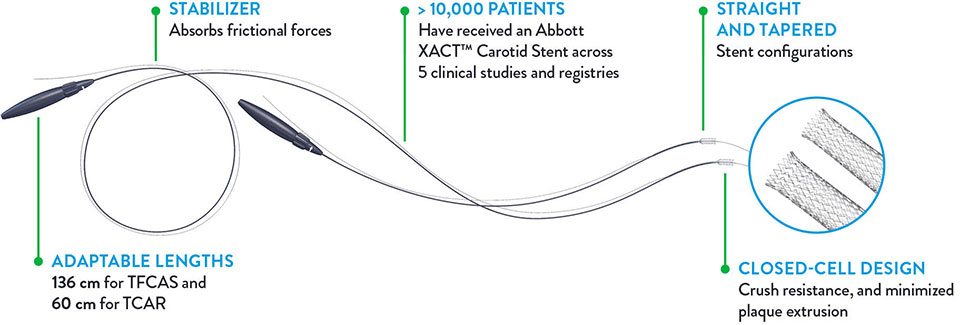
Optimized Stent Design for Carotid Artery Stenting (CAS) and Transcarotid Artery Revascularization (TCAR)
Unique Variable Cell Design
Provides targeted radial strength for carotid artery stenting (CAS), adapts to lesion location, and ensures optimized stent coverage to minimize plaque extrusion in transfemoral and transcarotid (TCAR) procedures.

Straight and Tapered Configurations
Tailored for diverse anatomical needs in carotid artery disease, supporting optimal vessel conformity and improving long-term patency.

Closed-Cell Construction
Enhances crush resistance, supports plaque stabilization, and reduces embolization risk when used with cerebral embolic protection devices.

Smooth and Controlled Deployment
Features an ergonomic handle with Freestyle™ stabilizer for precise, single-handed rotational deployment, ensuring accurate stent placement in carotid revascularization procedures.

Advanced Stent Cell Geometry
U- and S-shaped connectors improve stent flexibility, deliverability, and arterial conformability, while flared ends enhance stability and retrieval safety—reducing the risk of snagging with embolic protection filters during carotid artery stenting.


XACT™ Carotid Stent System Preparation and Deployment Video

*Data on file at Abbott unless otherwise noted.
References
- Lal, B. et al. Quality Assurance for Carotid Stenting in the CREST-2 Registry. Vol. 74 No. 25. 2019
MAT-2106474 v7.0
Important Safety Information
XACT™ Carotid Stent System

INDICATIONS
The XACT™ Carotid Stent System (XACT™), used in conjunction with the Emboshield™ family of Embolic Protection System is indicated for the improvement of the lumen diameter of carotid arteries in patients considered at high risk for adverse events from carotid endarterectomy who require percutaneous carotid angioplasty and stenting for occlusive artery disease and meet the criteria outlined below:
Patients with carotid artery stenosis (≥ 50% for symptomatic patients by ultrasound or angiography or ≥ 80% for asymptomatic patients by ultrasound or angiography), located between the origin of the common carotid artery and the intra-cranial segment of the internal carotid artery AND
Patients must have a reference vessel diameter ranging between 4.8 mm and 9.1 mm at the target lesion.
CONTRAINDICATIONS
Contraindications associated with angioplasty must be considered when using the XACT™ Carotid Stent System. These include, but are not limited to:
- Patients in whom anticoagulant and / or antiplatelet therapy is contraindicated.
- Patients with severe vascular tortuosity or anatomy that would preclude the safe introduction of the Guiding Catheter / Introducer Sheath, BareWire™ guide wire, Emboshield™ Delivery Catheter, Filtration Element, and / or Retrieval Catheter.
- Patients with a known hypersensitivity to nickel-titanium.
- Patients with uncorrected bleeding disorders.
- Lesions in the ostium of the common carotid artery.
WARNINGS
Only physicians who have received appropriate training and are familiar with the principles, clinical applications, complications, side effects and hazards commonly associated with carotid interventional procedures should use this device.
General
Refer to instructions supplied with all interventional devices to be used with the XACT™ Carotid Stent System for their intended uses, contraindications, and potential complications.
The safety and efficacy of the XACT™ Carotid Stent System has not been demonstrated with embolic protection systems other than the Emboshield™ Embolic Protection System.
The long-term performance (> 1 year) of the XACT™ Carotid Stent System has not been established.
As with any type of vascular implant, infection secondary to contamination of the stent may lead to thrombosis, pseudoaneurysm, or rupture.
Stenting across a major bifurcation may hinder or prevent future diagnostic or therapeutic procedures.
In patients requiring the use of antacids and / or H2-antagonists before or immediately after stent placement, oral absorption of antiplatelet agents (e.g. aspirin) may be adversely affected.
The appropriate antiplatelet and anticoagulation therapy should be administered pre- and post-procedure as suggested in these instructions. Special consideration should be given to those patients with recently active gastritis or peptic ulcer disease.
When multiple stents are required, stent materials should be of similar composition.
The safety and effectiveness of the XACT™ Carotid Stent System has NOT yet been established in patients with the characteristics noted below.
- Low to moderate risk for adverse events from carotid endarterectomy
- Previously placed stent in target artery.
- Total occlusion of target lesion.
- Angiographically visible thrombus.
- Carotid string sign (a tiny, long segment of contrast in the true lumen of the artery).
- Vessel anatomy precluding the use of the stent system or appropriate positioning of the embolic protection system.
- Presence of carotid artery dissection prior to initiation of the procedure.
- Evidence of a stroke within the previous 30 days.
- History of ipsilateral stroke with fluctuating neurologic symptoms within 1 year.
- History of intracranial hemorrhage within the past 3 months.
- Any condition that precluded proper angiographic assessment or made percutaneous arterial access unsafe, (e.g. morbid obesity, sustained systolic blood pressure > 180 mmHg).
- Contraindication to aspirin, or to clopidogrel AND ticlopidine, or stent material.
- History or current indication of bleeding diathesis or coagulopathy including thrombocytopenia or an inability to receive heparin in amounts sufficient to maintain an activated clot time at > 250 seconds.
- Hemoglobin (Hgb) < 8 gm / dl (unless on dialysis), platelet count < 50,000, INR > 1.5 (irreversible), or heparin-associated thrombocytopenia.
- Known cardiac sources of emboli.
- Atherosclerotic disease involving adjoining vessels precluding safe placement of the guiding catheter or sheath.
- Other abnormal angiographic findings that indicated the patient was at risk of a stroke due to a problem other than that of the target lesion, such as: ipsilateral arterial stenosis greater in severity than the target lesion, cerebral aneurysm, or arteriovenous malformation of the cerebral vasculature.
- Severe dementia.
- Life threatening allergy to contrast media that could not be treated.
- Pregnant patients or patients under the age of 18.
- Patients in whom femoral access is not possible.
- Patients with aneurysmal dilation immediately proximal or distal to the lesion.
The safety and effectiveness of concurrent treatment of lesions in patients with bilateral carotid artery disease have not been established.
PRECAUTIONS
Carefully inspect device components prior to use to verify that they have not been damaged and that the size, shape and condition are suitable for the procedure for which they are to be used. A device or access device which is kinked or damaged in any way should not be used. If pouch is damaged do not use.
Confirm the compatibility of the XACT™ Stent Delivery System with the interventional devices before actual use.
Precautions to prevent or reduce clotting should be taken when any interventional device is used. Flush or rinse all devices entering the vascular system with sterile isotonic heparinized saline prior to use.
Do not remove the stent from its delivery system as removal may damage the stent. The stent and delivery system are intended to be used in tandem. If removed, the stent cannot be put back on the delivery system.
The delivery system should not be used in conjunction with other stents.
To reduce the potential for the liberation of emboli during lesion crossing, the device should be carefully manipulated and not advanced against resistance.
During stent placement, 1.5 cm of vessel should be left between the distal margin of the stent and the Filtration Element. The stent delivery system should not contact the Filtration Element.
Venous access should be available during carotid stenting in order to manage bradycardia and / or hypotension by either pharmaceutical intervention or placement of a temporary pacemaker, if needed.
The device must only be flushed using the 3-ml syringe and flushing tip provided.
The outside diameter of the Outer Sheath is 5.7 Fr. An appropriate sized sheath / guiding catheter should be selected based on this diameter.
Do not use a prepared XACT™ Carotid Stent System if the stent is not fully constrained within the Delivery System.
Do not use if the stent is partially deployed.
If, after preparation, a gap between the catheter tip and the outer sheath exists, rotate the Deployment Actuator in an anti-clockwise direction until the gap is closed.
Advancement and deployment of the XACT™ Carotid Stent System should only be performed under fluoroscopic observation.
Do not advance any component, or section thereof, of the XACT™ Carotid Stent System against significant resistance. The cause of any resistance should be determined via fluoroscopy and remedial action taken.
Do not attempt to reposition the Delivery System once the stent has made contact with the vessel wall.
Do not torque the XACT™ Carotid Stent System.
If more than one stent is required to cover the lesion, or if there are multiple lesions, the distal lesion should be stented first, followed by stenting of the proximal lesion.
If overlap of sequential stents is necessary, the amount of overlap should be kept to a minimum.
MRI Information
Non-clinical testing has demonstrated that the XACT™ Carotid Stent is MR Conditional. It can be scanned safely under the conditions listed in the Instructions for Use.
Potential Adverse Effects
As reported in the literature, the following adverse events are potentially associated with carotid stents and embolic protection systems:
- Abrupt closure
- Allergic reactions
- Aneurysm
- Angina/Coronary ischemia
- Arteriovenous Fistula
- Bacteremia or septicemia
- Bleeding from anticoagulant or antiplatelet medications
- Bradycardia/arrhythmia
- Cerebral edema
- Cerebral hemorrhage
- Congestive Heart Failure
- Death
- Drug reactions
- Embolism (including air and device)
- Emergent or urgent Endarterectomy
- Fever
- Filter thrombosis / occlusion
- Fluid overload
- Groin hematoma, with or without surgical repair
- Hemorrhage or hematoma
- Hemorrhagic stroke
- Headache
- Hypotension
- Hyperperfusion syndrome
- Hypertension
- Infection / sepsis
- Ischemia / infarction of tissue / organ
- Myocardial Infarction
- Other conduction disturbances
- Pain and tenderness
- Pain, infection, or discomfort at the access site
- Pseudoaneurysm
- Renal failure / insufficiency
- Restenosis of the stented artery
- Seizure
- Stent deformation, collapse, fracture, movement of stent, possibly requiring emergency surgery
- Stent / filter entanglement / damage
- Stroke or other neurological complications
- Thromboembolic episodes
- Thrombophlebitis
- Total occlusion of the artery
- Transient ischemic attacks (TIAs)
- Vascular access complications (e.g. loss of pulse, femoral artery pseudoaneurysm and infection)
- Ventricular fibrillation
- Vessel dissection, rupture, or perforation
- Vessel thrombosis (partial blockage)
- Unstable angina pectoris
MAT-2006273 v3.0
XACT™ Transcarotid Stent System

INDICATIONS
The XACT™ Transcarotid Stent System (XACT™ TSS), used in conjunction with the ENROUTE‡ Transcarotid Neuroprotection System, is indicated for the improvement of the lumen diameter of carotid arteries in patients considered at high risk for adverse events from carotid endarterectomy who require percutaneous carotid angioplasty and stenting for occlusive artery disease and meet the criteria outlined below:
- Patients with carotid artery stenosis (≥ 50% for symptomatic patients by ultrasound or angiography or ≥ 80% for asymptomatic patients by ultrasound or angiography), located between the origin of the common carotid artery and the intra-cranial segment of the internal carotid artery AND
- Patients must have a reference vessel diameter ranging between 4.8 mm and 9.1 mm at the target lesion.
CONTRAINDICATIONS
Contraindications associated with angioplasty must be considered when using the XACT™ Transcarotid Stent System. These include, but are not limited to:
- Patients in whom anticoagulant and / or antiplatelet therapy is contraindicated.
- Patients with a known allergy or hypersensitivity to stent materials (nickel-titanium alloy) or contrast medium, who cannot be adequately premedicated.
- Patients with uncorrected bleeding disorders.
- Patients in whom carotid bifurcation is less than 5 cm above the clavicle (ENROUTE‡ Transcarotid Neuroprotection System only)
WARNINGS
Use of the device should be restricted to physicians or allied healthcare professionals under the direction of such physicians trained to the specifics of the device and to the Instructions for Use. Users must be knowledgeable of the current medical literature and appropriately trained on the principles, clinical applications, complications, side effects, and hazards commonly associated with carotid interventional procedures.
General
This device is designed and intended for single use only. Do not reuse, reprocess or resterilize. Reuse, reprocessing or resterilization may compromise the structural integrity of the device and / or delivery system and / or lead to device failure, which may result in patient injury, illness or death. Reuse, reprocessing or resterilization may also create a risk of contamination of the device and / or cause patient infection or cross-infection, including, but not limited to, the transmission of infectious diseases(s) from one patient to another. Contamination of the device and / or delivery system may lead to injury, illness or death of the patient.
DO NOT USE if the sterile pouch is damaged.
Keep dry. Keep away from sunlight. Do not expose to organic solvents or ionizing radiation.
Carefully inspect device components prior to use to verify that they have not been damaged and that the size, shape, and condition are suitable for the procedure for which they are to be used. A device or access device which is kinked or damaged in any way should not be used.
Do not use the product after the “Use by” Date specified on the label.
Refer to instructions supplied with all interventional devices to be used with the XACT™ Transcarotid Stent System for their intended uses, contraindications, and potential complications.
Confirm the compatibility of the XACT™ Transcarotid Stent Delivery System with the other interventional devices intended for use in the procedure. (Refer to the Instructions for Use for Materials Required)
The safety and efficacy of the XACT™ Transcarotid Stent System has not been demonstrated with embolic protection systems other than ENROUTE‡ Transcarotid Neuroprotection System. Refer to the Instructions for Use document for the embolic protection system that will be used for specific device instructions.
As with any vascular implant, infection secondary to contamination of the stent may lead to thrombosis, pseudoaneurysm, or rupture.
Stenting across a major bifurcation may hinder or prevent future diagnostic or therapeutic procedures.
Appropriate anti-platelet, anticoagulant, and, if necessary, vasodilator therapy must be used during the procedure. Anticoagulant therapy sufficient to maintain an Activated Clotting Time of at least 250 seconds for the duration of the procedure is recommended.
The appropriate antiplatelet and anticoagulation therapy should be administered pre- and post-procedure as suggested in these instructions. Special consideration should be given to those patients with recently active gastritis or peptic ulcer disease.
In patients requiring antacids and / or H2-antagonists before or immediately after stent placement, oral absorption of antiplatelet agents (e.g., aspirin) may be adversely affected.
When multiple stents are required, stent materials should be of similar composition.
The safety and effectiveness of the XACT™ Transcarotid Stent System has NOT yet been established in patients with the characteristics noted below:
- Low to moderate risk for adverse events from carotid endarterectomy.
- Previously placed stent in target artery.
- Total occlusion of the target lesion.
- Angiographically visible thrombus.
- Carotid string sign (a tiny, long segment of contrast in the true lumen of the artery).
- Other abnormal angiographic findings that indicate the patient is at risk of a stroke due to a problem other than that of the target lesion, such as: ipsilateral arterial stenosis greater in severity than the target lesion, cerebral aneurysm, or arteriovenous malformation of the cerebral vasculature.
- Vessel anatomy precluding the use of the stent system or appropriate positioning of the embolic protection system.
- Presence of carotid artery dissection prior to initiation of the procedure.
- Evidence of a stroke within the previous 30 days.
- History of ipsilateral stroke with fluctuating neurologic symptoms within 1 year.
- History of intracranial hemorrhage within the past 3 months.
- Any condition that precluded proper angiographic assessment or made percutaneous arterial access unsafe (e.g., morbid obesity, sustained systolic blood pressure > 180 mmHg).
- History or current indication of bleeding diathesis or coagulopathy, including thrombocytopenia or an inability to receive heparin in amounts sufficient to maintain an activated clot time at > 250 seconds.
- Hemoglobin (Hgb) < 8 gm/dl (unless on dialysis), platelet count < 50,000, INR > 1.5 (irreversible), or heparin-associated thrombocytopenia.
- Known cardiac sources of emboli.
- Atherosclerotic disease involving adjoining vessels (i.e., ostial common carotid artery) precluding safe placement of the arterial sheath.
- Severe dementia.
- Pregnant patients or patients under the age of 18.
- Patients in whom transcarotid access is not possible.
- Patients with aneurysmal dilation immediately proximal or distal to the lesion.
The safety and effectiveness of concurrent treatment of lesions in patients with bilateral carotid artery disease have not been established.
Overstretching of the artery may result in rupture and life-threatening bleeding.
Device insertion should be performed slowly to minimize the risk of air entrainment.
During the insertion of Rapid Exchange catheters through the arterial sheath, careful handling is required to ensure that air is not drawn into the hemostatic valve. Therefore, flushing of contrast media (or other fluids) is recommended before or after insertion of the catheter, but not while the catheter is within the hemostatic valve.
Do not advance any component of the XACT™ Transcarotid Stent Delivery System against significant resistance. The cause of any resistance should be determined via fluoroscopy, and remedial action should be taken.
Maintain continuous flush while removing and reinserting devices on the guide wire. Perform all exchanges slowly to prevent air embolism or trauma to the artery.
Implanting a stent may lead to dissection of the vessel distal and / or proximal to the stent. It may cause acute vessel closure requiring additional intervention (carotid endarterectomy, further dilatation, or placement of additional stents).
The stent may cause thrombus, distal embolization, or may migrate from the site of the implant down the arterial lumen. Appropriate sizing of the stent to the vessel is required to reduce the possibility of stent migration. In the event of thrombosis of the expanded stent, thrombolysis and percutaneous transluminal angioplasty (PTA) should be attempted. (Refer to the Instructions for Use for stent sizing)
In the event of complications such as infection, pseudoaneurysm, or fistulization, surgical removal of the stent may be required.
Caution should be used if pre-dilating the lesion without embolic protection as this may increase the risk of an adverse outcome.
Ensure optimal positioning of the stent prior to deployment. Once deployment is initiated, the stent cannot be repositioned or recaptured. Stent retrieval methods (use of additional wire, snares, and / or forceps) may result in additional trauma to the carotid vasculature and / or the vascular access site. Complications may include death, stroke, bleeding, hematoma, or pseudoaneurysm.
To reduce the potential of emboli during lesion crossing, the device should be carefully manipulated and not advanced against resistance.
Do not attempt to reposition the delivery system once the stent has made contact with the vessel wall.
Do not torque the XACT™ Transcarotid Stent System.
If resistance is met during delivery system introduction, the system should be withdrawn and another system used.
Should unusual resistance be felt at any time during removal of the Delivery System post-stent implantation, the entire system should be removed together with the transcarotid arterial sheath as a single unit.
Persons with known history of allergies to any of the components of the XACT™ Transcarotid Stent System listed below may suffer an allergic reaction to this device. Prior to use on the patient, the patient should be counselled on the materials contained in the device, and a thorough history of allergies must be discussed. The delivery system contains stainless steel, polyether block amide, polytetrafluoroethylene, polyamide, silicone, polyethylene, polyetheretherketone, polyimide, tungsten, barium sulphate, and platinum-iridium alloy.
PRECAUTIONS
Precautions to prevent or reduce clotting should be taken when any interventional device is used. Flush or rinse all devices entering the vascular system with sterile isotonic heparinized saline prior to use.
The device must only be flushed using the 3 ml syringe and flushing tip provided.
Do not remove the stent from its delivery system, as removal may damage the stent. The stent and delivery system are intended to be used in tandem. If removed, the stent cannot be put back on the delivery system.
The delivery system should not be used in conjunction with other stents.
Femoral venous access is available during carotid stenting to manage potential hemodynamic instability (i.e., bradycardia and / or hypotension) by either pharmaceutical intervention or placement of a temporary pacemaker, if needed.
For use via the transcarotid artery revascularization (TCAR) approach, the XACT™ Transcarotid Stent System must be used with the transcarotid arterial sheath to main adequate support of the 0.014” (0.36mm) guide wire throughout the procedure.
The outside diameter of the Distal Outer Sheath is 5.7 Fr. It is intended to be used with the arterial sheath included with the ENROUTE‡ Transcarotid Neuroprotection System.
Do not use if the stent is partially deployed within the stent delivery system.
If, after preparation, a gap between the catheter tip and the outer sheath exists, rotate the Deployment Actuator in an counter-clockwise direction until the gap is closed.
Advancement and deployment of the XACT™ Transcarotid Stent System should only be performed under fluoroscopic observation.
If more than one stent is required to cover the lesion, or if there are multiple lesions, the most distal lesion should be stented first, followed by the stenting of the proximal lesion. Stenting in this order obviates the need to cross the proximal stent for placement of the distal stent and reduces the chance of dislodging stents that have already been placed.
If an overlap of sequential stents is necessary, the amount of overlap should be kept to a minimum. In no instance, should more than 2 stents ever overlap.
Do not expose the delivery system to organic solvents (e.g., alcohol) as the device’s structural integrity and / or function may be impaired.
Care must be exercised when crossing a newly deployed stent with other interventional devices to avoid disrupting the stent geometry and placement of the stent.
The deployment actuator should not be rotated before the undeployed stent within the RX delivery system has been positioned at its intended deployment location.
Do not attempt to pull a partially expanded stent back through the arterial sheath; dislodgment of the stent from the delivery system may occur.
MRI INFORMATION
 MR Conditional MR ConditionalMRI Safety Information Nonclinical testing has demonstrated that the XACT Carotid Stent is MR Conditional for single and overlapping lengths up to 75 mm in length. A person with the XACT Carotid Stent may be safely scanned under the following conditions. Failure to follow these conditions may result in injury. | |
| Device Name | XACT™ Carotid Stent |
| Static Magnetic Field Strength (B0) | 1.5 or 3 Tesla |
| Maximum Spatial Field Gradient | 3000 gauss/cm (30 T/m) |
| Maximum Gradient Slew Rate | 200 T/m/s per axis |
| RF Exitation | Circularly Polarized (CP) |
| RF Transmit Coil Type | There are no Transmit Coil restrictions |
| Operating Mode | Normal Operating Mode |
| Maximum MR System reported whole-body-averaged specific absorption rate (SAR) | 2.0 W/kg (normal operating mode) |
| Scan Duration | 60 minutes of continuous RF scanning with 2 W/kg whole body average SAR |
| MR Image Artifact | The presence of this implant may produce an image artifact |
The XACT™ Carotid Stent should not migrate in this MRI environment. Nonclinical testing at field strengths greater than 3 Tesla has not been performed to evaluate stent migration or heating. MRI at 1.5 or 3 Tesla may be performed immediately following the implantation of the XACT Carotid Stent.
POTENTIAL ADVERSE EVENTS
As reported in the literature, the following adverse events are potentially associated with carotid stents and embolic protection systems:
- Allergic reaction or hypersensitivity to contrast agent, anesthesia, stent materials (nitinol, nickel, titanium), and drug reactions to anticoagulation, or antiplatelet drugs
- Vascular access complications which may require transfusion or vessel repair, including:
- Catheter site reactions
- Bleeding (ecchymosis, oozing, hematoma, hemorrhage, retroperitoneal hemorrhage)
- Arteriovenous fistula, pseudoaneurysm, aneurysm, dissection, perforation / rupture, and laceration
- Embolism (air, tissue, plaque, thrombotic material, or device)
- Thrombophlebitis
- Target artery complications which may require additional intervention, including:
- Total occlusion or abrupt closure
- Arteriovenous fistula, pseudoaneurysm, aneurysm, dissection, perforation / rupture
- Embolism (air, tissue, plaque, thrombotic material or device)
- Artery, stent, or filter thrombosis / occlusion thrombosis
- Stenosis or restenosis
- Vessel spasm or recoil
- Cardiac arrhythmias (including conduction disorders, atrial and ventricular arrhythmias)
- Cardiac ischemic conditions (including myocardial ischemia, myocardial infarction, and unstable or stable angina pectoris)
- Stroke / cerebrovascular accident (CVA) and transient ischemic attack (TIA)
- System organ failure:
- Cardio-respiratory arrest
- Cardiac failure
- Cardiopulmonary failure (including pulmonary edema)
- Renal failure / insufficiency
- Shock
- Bleeding
- Blood cell disorders, including heparin-induced thrombocytopenia (HIT) and other coagulopathy
- Hypotension / hypertension
- Peripheral nerve injury
- Other ischemic conditions / infarct
- Infection – local and systemic (including post-procedural)
- Nausea and vomiting
- Chest pain
- Dyspnea
- Edema / cerebral edema and fluid overload
- Fever
- Pain, including headache
- Hyperperfusion syndrome
- Other neurologic and systemic complications
- Seizure
- Cerebral hemorrhage
- Death
- Device-related complications which may require additional intervention, including:
- Detachment and / or implantation of a component of the system
- Stent / damage
- Stent malposition
- Stent migration / embolization
- Emergent or urgent endarterectomy surgery (CEA)
MAT-2408573 v1.0
