Real-World Evidence Shows ICMs Yield Higher Rates of Atrial Fibrillation Diagnosis After Cryptogenic Stroke
Abbott Cardiac Rhythm Management | September 20, 2023

Real-world evidence from a U.S. nationwide study shows that insertable cardiac monitoring results in higher rates of atrial fibrillation (AF) diagnosis and oral anticoagulation implementation compared to external cardiac monitoring after cryptogenic stroke (CS).
While the American Heart Association and American Stroke Association guidelines recommend long-term cardiac monitoring for cryptogenic stroke patients, there are many options for cardiac monitoring. The impact of monitoring for AF detection in CS patients has mostly been evaluated in randomized control trials, not real-world populations and practice.
The featured real-world evidence (RWE) data comes from a study of U.S. Medicare beneficiaries diagnosed with cryptogenic stroke who either received an insertable cardiac monitor (ICM) or external cardiac monitor (ECM) post-stroke. The results were presented at the Asia Pacific Heart Rhythm Society in Singapore last winter and a full manuscript is now available in EP Europace. The study results compare AF detection and oral anticoagulation (OAC) rates for patients diagnosed with CS with long-term ICMs versus short-term ECMs.
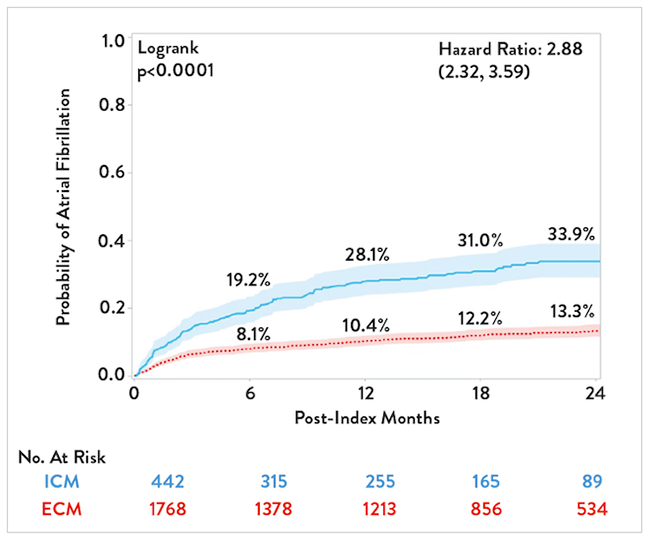
The results concluded AF detection rate was 33.9% among ICM patients compared to 13.3% among ECM patients at two years. The adjusted hazard ratio demonstrates a three times higher rate of AF detection with an ICM compared to an ECM alone (Figure 1). As shown in Figure 1, ICM patients are diagnosed with AF at a faster rate than ECM patients.1
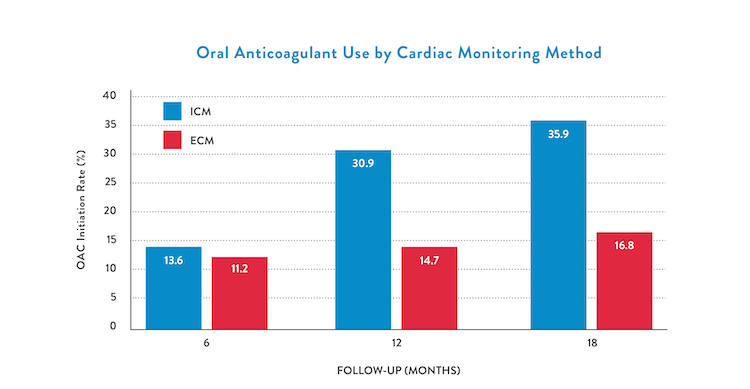
Further results demonstrate the OAC rate was 35.9% among ICM patients compared to 16.8% among ECM patients at 1.5 years (p<0.0001). Figure 2 shows that ICM patients had a significant three times higher rate of OAC initiation when compared to ECM alone (2.91, 95 percent CI: 2.28, 3.72).
AF is known to be prevalent in more than one-fourth of patients with recent ischemic stroke2, and there is a 50% likelihood of death for AF-related strokes within one year after a stroke event.3 Long-term monitoring is reported to detect AF in approximately 30% of CS patients.4 The featured real-world evidence demonstrates ICMs detect AF three times faster than ECM methods for CS patients, thereby allowing early initiation of OAC, ultimately reducing the risk of recurrent stroke.3
Endpoints for the study included AF detection defined by at least one inpatient or two hospital outpatient visits or physician claims with AF diagnosis codes in the first or second positions of the claim. The secondary endpoint was an OAC prescription fill.
More than 2,000 Medicare FFS patients were implanted with a de novo Abbott ICM or provided an ECM after a CS diagnosis between November 2017 and December 2019. Patients were propensity matched one-to-four with the larger group representing ECMs as the control group. Study selection criteria included hospitalization with ischemic stroke in the three months prior to de novo device use with no previous history of atrial arrhythmias, no previous history of a cardiac implantable electronic device (CIED) or OAC use. Criteria also included continuous Medicare FFS, as well as prescription drug coverage one year prior to index monitoring.
Cohorts were additionally matched by demographics (age, sex, race/ethnicity), stroke hospitalization characteristics and comorbidities.
Abbott ICMs provide diagnostic solutions for patients after ischemic stroke. Learn more about the featured real-world evidence.
™ Indicates a trademark of the Abbott group of companies.
REFERENCES
- Boriani G, Auricchio A, Botto GL, et al. Insertable Cardiac Monitoring Results in Higher Rates of Atrial Fibrillation Diagnosis and Oral Anticoagulation Prescription after Ischaemic Stroke. EP Europace. 2023; euad212, https://doi.org/10.1093/europace/euad212.
- Sposato LA, Chaturvedi S, Hsieh C-Y, Morillo CA, Kamel H. Atrial Fibrillation Detected After Stroke and Transient Ischemic Attack: A Novel Clinical Concept Challenging Current Views. Stroke. 2022;53(3):e94-e103. doi:10.1161/ STROKEAHA.121.034777
- Benjamin EJ, Wolf PA, D’Agostino RB, Silbershatz H, Kannel WB, Levy D. Impact of Atrial Fibrillation on the Risk of Death: the Framingham Heart Study. Circulation. 1998;98(10):946-952. doi:10.1161/01.cir.98.10.946
- Kloosterman EM, Rosman JZ, Berkowitz EJ, Rosenbaum M, Wettenstein ZA. Treatment of Cryptogenic Stroke Patients with Atrial Fibrillation Detected by Insertable Cardiac Monitors Reduces Recurrent Stroke Risk to Background Levels. The Journal of Innovations in Cardiac Rhythm Management. 2021;12(12):4812-4817. doi:10.19102/ icrm.2021.121204

MAT-2310025 v2.0
