Abbott Implantable Cardioverter Defibrillators (ICDs) and Cardiac Resynchronization Therapy Defibrillators (CRT-Ds) are built with exclusive algorithms proven to deliver better patient outcomes that have the potential to save more lives. It is this type of innovation that drives us at Abbott to personalize therapy and restore quality of life for patients.
Abbott's CRT-D and Insertable Cardioverter Defibrillator platforms are designed with a focus on providing the best outcome for the patient. See the story of Rob, a navy veteran, who experienced cardiac arrest while in the best shape of his life.
His heart had to be shocked five times on the way to the hospital and doctors did not believe he would make it. After being implanted with a Gallant™ Implantable Cardioverter Defibrillator, Rob, and his family feel confident that he is now receiving the therapy he needs to stay alive.


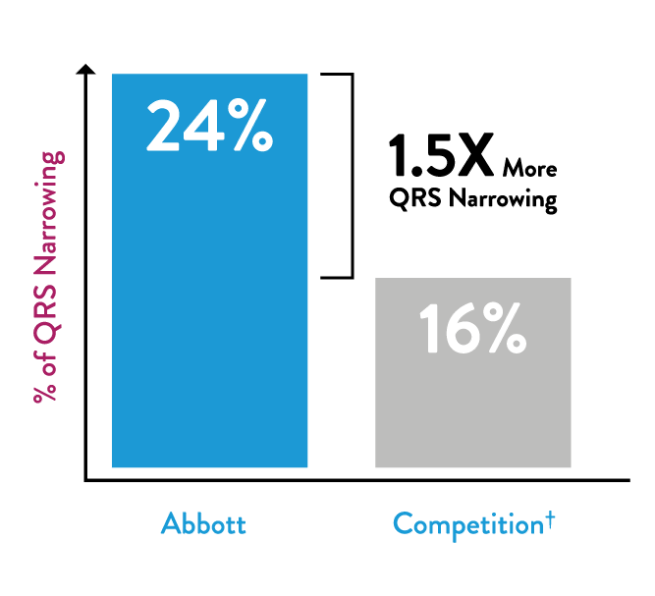
SyncAV CRT Technology provides the most QRS narrowing options at implant for patients. QRS narrowing after CRT implantation allows improved mortality. In patients with LBBB, QRS narrowing after CRT implant is associated with 2x lower mortality.
Published rate of QRS Narrowing at implant


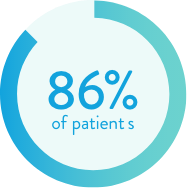
VF Therapy Assurance is the only technology to provide an additional safety net for difficult to detect ventricular arrhythmias. Without VF Therapy Assurance, ventricular tachyarrhythmias with low and varying signal amplitudes may not be successfully identified.5
who received HV therapy due to VF Therapy Assurance's enhanced detection would have been otherwise
untreated for potentially life-threatening arrhythmias
>800 PATIENTS ANNUALLY WORLDWIDE
with challenging arrhythmias
could have their lives saved
because of VF Therapy Assurance.6,7


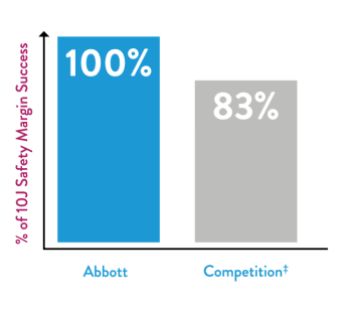
DeFT Response Technology is the industry's most flexible option for the management of high DFT. The algorithm supports a 10J shock safety margin for patients.8
Abbott’s 1.5T and 3T MRI ready solutions* ensure no loss of CRT therapy for your patients during full-body scans and allows for programming of an MRI timeout.**


Rx Only
Intended Use: The Implantable Cardioverter Defibrillator (ICD) and Cardiac Resynchronization Therapy Defibrillator (CRT-D) devices are intended to provide ventricular antitachycardia pacing and ventricular cardioversion/defibrillation. The CRT-D devices are also intended to resynchronize the right and left ventricles.
The myMerlinPulse™ mobile application is intended for use by people who have an Abbott Medical implanted heart device and access to a mobile device. The app provides remote monitoring capability of the implanted heart device by transmitting information from the patient’s implanted heart device to the patient’s healthcare provider.
Indications: The ICD and CRT-D devices are indicated for automated treatment of life-threatening ventricular arrhythmias. CRT-D devices are also indicated to treat symptoms in patients who have congestive heart failure with ventricular dyssynchrony.
In addition, dual chamber ICD and CRT-D devices with the AT/AF detection algorithm are indicated in patients with atrial tachyarrhythmias or those patients who are at significant risk of developing atrial tachyarrhythmias.
MR Conditional ICDs and CRT-Ds are conditionally safe for use in the MRI environment when used in a complete MR Conditional system and according to instructions in the MRI-Ready Systems manual. Scanning under different conditions may result in severe patient injury, death or device malfunction.
The myMerlinPulse™ mobile application is indicated for use by patients with supported Abbott Medical implanted heart devices.
Contraindications: Contraindications for use of the pulse generator system include ventricular tachyarrhythmias resulting from transient or correctable factors such as drug toxicity, electrolyte imbalance, or acute myocardial infarction.
The myMerlinPulse™ mobile application is contraindicated for use with any implanted medical device other than supported Abbott Medical implanted heart devices.
Adverse Events: Possible adverse events associated with the implantation of the pulse generator system include the following: Arrhythmia (for example, accelerated or induced), Bradycardia, Cardiac or venous perforation, Cardiac tamponade, Cardiogenic shock, Death, Discomfort, Embolism, Endocarditis, Erosion, Exacerbation of heart failure, Excessive fibrotic tissue growth, Extracardiac stimulation (phrenic nerve, diaphragm, pectoral muscle), Extrusion, Fluid accumulation within the device pocket, Formation of hematomas, cysts, or seromas, Heart block, Hemorrhage, Hemothorax, Hypersensitivity, including local tissue reaction or allergic reaction, Infection,Keloid formation, Myocardial damage, Nerve damage, Occlusion/Thrombus, Pericardial effusion, Pericarditis, Pneumothorax, Pulmonary edema, Syncope, Thrombosis, Valve damage. Complications reported with direct subclavian venipuncture include pneumothorax, hemothorax, laceration of the subclavian artery, arteriovenous fistula, neural damage, thoracic duct injury, cannulation of other vessels, massive hemorrhage and rarely, death. Among the psychological effects of device implantation are imagined pulsing, depression, dependency, fear of premature battery depletion, device malfunction, inappropriate pulsing, shocking while conscious, or losing pulse capability. Possible adverse device effects include complications due to the following: , Abnormal battery depletion, Conductor fracture, Device-programmer communication failure, Elevated or rise in defibrillation/cardioversion threshold, Inability to defibrillate or pace, Inability to interrogate or program due to programmer or device malfunction, Incomplete lead connection with pulse generator, Inhibited therapy including defibrillation and pacing, Inappropriate therapy (for example, shocks and antitachycardia pacing [ATP] where applicable, pacing), Interruption of function due to electrical or magnetic interference, Intolerance to high rate pacing (for example dyspnea or discomfort), Lead abrasion, Lead fracture, Lead insulation damage, Lead migration or lead dislodgement, Loss of device functionality due to component failure, Pulse generator migration, Rise in DFT threshold, Rise in pacing threshold and exit block, Shunting of energy from defibrillation paddles, System failure due to ionizing radiation. Additionally, potential adverse events associated with the implantation of a coronary venous lead system include the following: Allergic reaction to contrast media, Breakage or failure of implant instruments, Prolonged exposure to fluoroscopic radiation, Renal failure from contrast media used to visualize coronary veins. Refer to the User’s Manual for detailed intended use, indications, contraindications, warnings, precautions and potential adverse events.
No potential adverse events have been identified with use of the myMerlinPulse™ mobile application.
* For additional information about specific MR Conditional ICDs and leads, including scan parameters, warnings, precautions, adverse conditions to MRI scanning, and potential adverse events, please refer to the Abbott MRI Ready Systems Manual at medical.abbott/manuals.
** No Loss of CRT therapy only applicable for model numbers CDHFA500Q and CDHFA600Q
† Competition defined as LV Only and BiV Simultaneous pacing modes. Modes 1 and IV of the referenced JAHA data.
‡ Fixed-tilt group of patients with competitive devices only achieved 83% success for maintaining a 10J safety margin
MAT-2112854 v3.0
You are about to enter an Abbott country- or region-specific website.
Please be aware that the website you have requested is intended for the residents of a particular country or countries, as noted on that site. As a result, the site may contain information on pharmaceuticals, medical devices and other products or uses of those products that are not approved in other countries or regions
Do you wish to continue and enter this website?
MAT-2305078 v1.0